NKC Health, (North Kansas City Hospital and Meritas), which together provide hospital, primary and specialty care in the Kansas City Northland, sent a contract termination notice to Blue Cross and Blue Shield of Kansas City (Blue KC), terminating its hospital and physician network participation agreements in all Blue KC networks as of June 1, 2026. This means NKC Health will remain in Blue KC networks until 11:59 p.m. on May 31, 2026.
Please know that right now, nothing is changing for you as a Blue KC member.
NKC Health remains in network until the termination date, and you will not see changes to coverage or your physicians or services at NKC Health hospital, health centers, and clinics. This information will be updated if an agreement cannot be reached by June 1, 2026. Please continue to check this website for updates.
As always, we remain willing to engage in good faith negotiations with NKC Health to continue their participation in all Blue KC networks.
What happened?
NKC Health sent a termination notice to Blue KC on March 2, 2026, terminating its hospital and physician network participation agreements in all Blue KC networks effective June 1, 2026.
NKC Health has stated that “our reimbursement from Blue KC has stayed the same since 2021,” and that is not accurate. The reimbursement for many NKC Health services has increased each year since 2021. Blue KC was surprised to receive NKC Health’s termination notice since we have offered contract rate increases to NKC Health during the past five years, however the offers were not accepted nor countered.
What is Blue KC doing?
Blue KC knows healthcare must be affordable to be accessible. We are always willing to engage in good faith negotiations with NKC Health to continue their participation in all Blue KC networks. As Kansas City’s local, not-for-profit health insurer, we are deeply committed to our mission of providing affordable access to healthcare and improving the health of our members.
What happens if NKC Health and Blue KC do not reach an agreement prior to the termination date?
If NKC Health and Blue KC do not reach an agreement prior to 11:59 p.m. on May 31, 2026, NKC Health will no longer be in Blue KC networks. We realize the difficulty this may cause for members who use NKC Health services, and we are dedicated to finding in-network solutions for them. For more details, please see the FAQs below.
On and after June 1, 2026, all Blue KC members will still be able to receive emergency care at NKC Health emergency departments. Emergency care is always covered at the in-network cost for members.
If your health plan includes out-of-network benefits, you will be able to receive healthcare at NKC Health but your out-of-pocket expenses will likely increase.
If your health plan does not include out-of-network benefits, for non-emergency care, Blue KC will work with members to find an alternative in-network provider to continue your care and cover medically necessary services.
Medicare Supplement members can go to any provider who accepts Medicare, so the termination does not apply to them.
We also encourage members to use Blue KC’s Find Care tool on MyBlueKC.com to find in-network physicians and other providers.
Members should use in-network healthcare facilities to ensure they have fewer out-of-pocket expenses and receive the most value from their insurance plan. If members don’t have internet access, they can call the customer service number on their member ID card for help.
If NKC Health leaves Blue KC’s networks on June 1, 2026, Blue KC members will still have in-network access to the following hospitals:
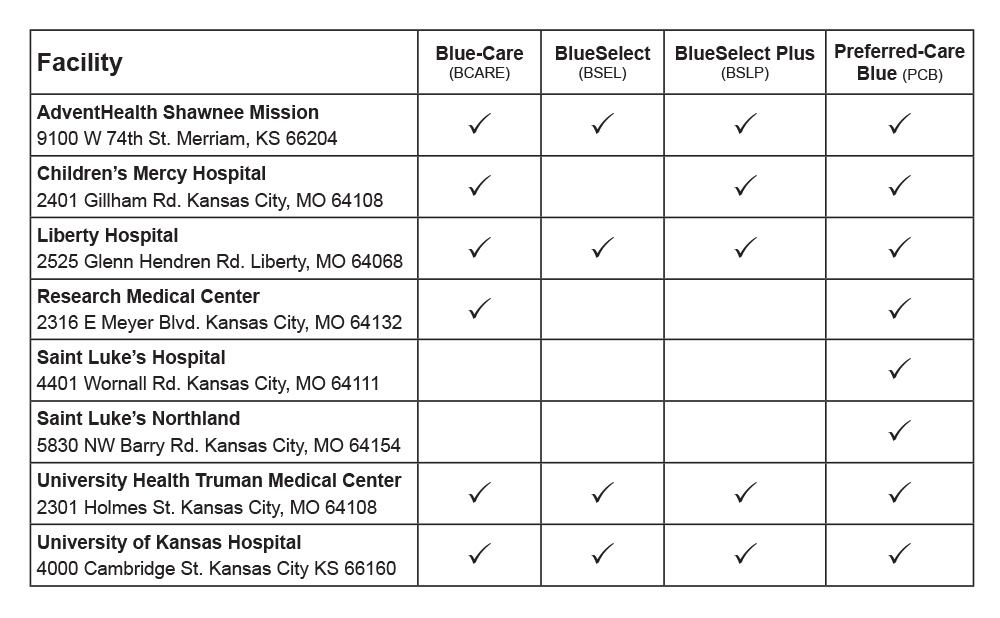
We understand that NKC Health’s decision to terminate their contract with Blue KC is especially concerning if you’re currently receiving care at NKC Health.
Affected members who are in an ongoing course of treatment may be eligible to continue care with their provider for up to 90 days at the in-network level. This is sometimes called “continuity of care” or “continuing care.”
Continuing care patients are defined as individuals who, with respect to a provider or facility, are at least one of the following:
- Undergoing treatment from the provider or facility for a serious and complex condition, including mental health and substance use disorder, defined as:
- In the case of an acute illness, a condition that is serious enough to require specialized medical treatment to avoid the reasonable possibility of death or permanent harm.
- In the case of a chronic illness or condition, a condition that is: life-threatening, degenerative, potentially disabling, or congenital; and requires specialized medical care over a prolonged period of time.
- Undergoing a course of institutional or inpatient care from the provider or facility.
- Scheduled to undergo nonelective surgery from the provider or facility, including receipt of postoperative care from such provider or facility with respect to such a surgery.
- Pregnant and undergoing treatment for pregnancy from the provider or facility.
- Terminally ill and receiving treatment for such illness from the provider or facility.
When a hospital, health system, or healthcare provider contracts with a Blue KC network, they are considered in-network and have signed a contract to charge rates negotiated between the parties, which can help keep your out-of-pocket costs lower and your care more affordable.
In-network: When a doctor or other healthcare provider joins a Blue KC network, they are considered in-network and have signed a contract to accept rates negotiated by Blue KC and the provider.
Out-of-network: A provider who has not signed a contract agreeing to negotiated rates is an out-of-network provider. Depending on the terms of your health plan, out-of-network doctors may only be partially covered by your plan, or not at all.
Blue KC offers a “Find Care” or provider lookup tool where you can see which doctors and hospitals accept your insurance plan. You can also call the customer service number on your member ID card.
Provider reimbursement rates are payments healthcare providers receive from insurance companies for the services providers give to our members. It is our goal to keep our local hospital and health systems strong, while helping to ensure healthcare is affordable and accessible for our members. There are many factors that may impact provider reimbursement. Our goal is fair reimbursement for providers with affordability for members and employer groups.
Discussions between Blue KC and hospitals and health systems typically start months in advance of their contract renewal dates. As a not-for-profit health plan, we approach every negotiation as a partnership built on mutual respect and shared goals. When we work with our hospital and health system partners to negotiate payment rates, we strive for transparent and collegial discussions that prioritize our members’ health and ability to access affordable, high-quality healthcare services.
As a not-for-profit health plan, Blue KC reinvests back into the community and its services. This allows Blue KC to focus on providing high-quality, sustainably affordable health coverage for its members. During provider negotiations, this commitment guides the organization’s efforts to balance fair reimbursement for providers with affordability for members and employer groups.
Blue KC is happy to answer additional questions about your health insurance or the network participation status of your provider. Please call our customer service team at the number listed on your member ID card.